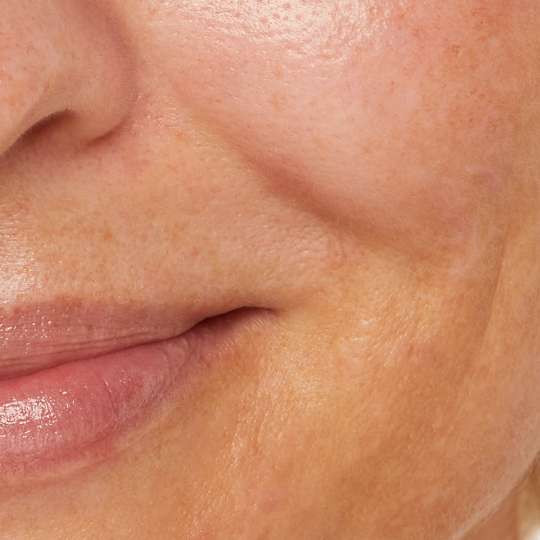

What is melasma?
Commonly referred to as “pregnancy mask”, melasma is a skin condition whereby large patches of pigmentation appear on the surface of your complexion. Compared to other types of hyperpigmentation, like age spots or freckles, melasma is much larger. It is flat to the skin and not raised.
“Melasma is symmetrical pigmentation that develops frequently on the face, the forehead, upper cheeks and upper lip,” adds consultant dermatologist Dr Justine Hextall. “It can develop at different levels in the skin and can be superficial or deep. Melasma can be difficult to treat and frequently recurs.”
You are more likely to develop melasma if:
-
You are aged between 20 and 40 years old
-
You have a darker skin tone or tan easily
-
Are pregnant or peri-menopausal
-
Someone in your immediate family has melasma
What causes melasma?
Melasma occurs when the melanocytes, the skin cells that create melanin (which gives our skin its pigment) go into overdrive. They are effectively working far too hard, creating far more melanin than the skin needs. Think of it like a few bees buzzing around a garden compared to a whole swarm of them collecting in one place.
Melasma is not triggered by just one thing, but it’s a combination of factors that cause the melanocytes to behave in this way. “Melasma is usually caused by a combination of hormones, such as oestrogen, alongside UV exposure,” explains Dr Hextall. “It can have a genetic element and is common in pregnancy.”
The reason for its prominence in pregnancy? “The increase in hormones oestrogen and progesterone, and also the melanocyte stimulating hormone (MSH), during pregnancy is thought to trigger melasma,.” says Dr Hextall. Especially when you combine this cocktail of hormones with UV exposure from the sun.
Melasma is often common during perimenopause, when hormones also fluctuate at a rollercoaster rate and oestrogen can surge before depleting. If you are taking hormone replacement therapy (HRT), this will add extra oestrogen into your system, which can also trigger melasma. During this time melasma may also appear on the arms, as well as the face.
How can you prevent melasma?
Melasma is, in most cases, connected to hormones, making it tricky to prevent. For example, there is no way to avoid the hormonal fluctuations that occur during pregnancy.
What you can do is make sure you are wearing a broad spectrum sunscreen all year round – even on cloudy days. This will shield skin from both UVB rays, which tend to cause burning, and UVA rays, which are responsible for the majority of premature ageing. UVA rays are able to penetrate through clouds, and even glass, so it’s important to be vigilant.
Adding an antioxidant serum into your daily skincare routine will help to support your SPF, by adding extra protection from free radicals (skin-destroying molecules that come from UV rays, as well as things like pollution). Think of it like adding an extra layer of clothing on a rainy day, such as a waterproof coat as well as an umbrella. Vitamin C is one of the most popular antioxidants to be applied topically, and you can supercharge its benefits by taking in supplement form too.
How to treat melasma
It is possible that melasma will retreat and fade on its own. In the case of “pregnancy mask” melasma, once your hormones have settled down, there is a chance the melasma may reduce too. You may also find that it is only more prominent in the summer months, and barely noticeable during the winter. Unfortunately, that is not always the case, and melasma can be difficult to shift from your skin.
Cosmetic strengths of alpha-hydroxy acids and vitamin C may help to slightly lessen its appearance, but won’t be enough to make long-term change. In a clinic, under the care of a dermatologist, there are more options available. But even then, it’s important to tread carefully.
“Melasma treatment needs very careful assessment, as some treatments may make pigmentation worse,” explains Dr Hextall. “Sometimes skin lightening creams may be used as a short-term treatment. There is also new evidence of the use of tranexamic acid both orally and topically in the treatment of melasma.”
Outside of topicals, you may be a good candidate for procedures such as chemical peels, microneedling and laser treatments. If this is the case, you will need to be extra careful in the sun to stop the melasma from returning. Remember, do your research thoroughly first and only go ahead with treatment if you feel totally comfortable and confident in the practitioner.
Read, watch and be inspired...



